
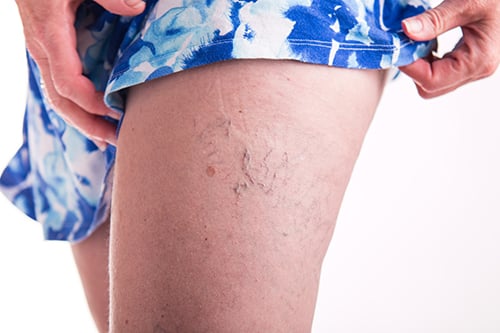
Spider veins are small dilated blood vessels that can be red or bluish and appear predominantly on the legs, though occasionally on the face and chest as well. They can be individual vessels or can appear in a sunburst pattern; sometimes they are localized to a small area, and other times they can extend over a wide area of the skin and be quite unattractive.
Varicose veins are much larger dilated vessels, which are often raised above the skin surface and can cause discomfort after prolonged standing or sitting.
While both types of vessels carry blood, it is generally safe to eliminate them, as the blood will find new pathways over time.
The cause of spider veins is not known, but in many cases, they seem to run in families. Spider veins are more common in women, and hormonal influences, such as estrogen and progesterone, may play a role. Also, puberty, birth control pills, pregnancy, or hormone replacement therapy may be the cause of their development. They can also appear after wearing tight garments on the legs or an injury. Sometimes they look like a flare around an area of larger varicose veins. People with lifestyles that involve prolonged standing or airplane travel seem to develop spider veins more frequently.
While they can’t always be prevented, wearing prescription support hose if you are at risk will undoubtedly give you the most significant chance of avoiding them. We recommend that pregnant women speak with their obstetricians to find a type of hose that is comfortable and effective.
Sclerotherapy is a procedure that has been safely used for more than 80 years to treat spider veins. It involves an injection of one or several types of solutions directly into the small vessels to irritate the vessel walls and cause them to seal up. Over time, the vessels turn into small areas of scar tissue that eventually become barely visible. Most of the time, each small vessel will need several injections sessions, generally three to four, separated by about a month. All of the areas can be injected at each session. Interestingly, it is not uncommon for the larger, reticular vessels to disappear more efficiently than the tiny little spider veins. When large varicose veins are present, your physician may have you evaluated by a vascular surgeon to see whether another type of laser ablation of those veins is necessary before embarking on the smaller spider veins. A variety of different solutions can be used, including sotradecol, polidocanol, and glycerin. Your physician will decide on a treatment plan that is right for you.
Any treatment that has survived the test of time, such as sclerotherapy, must be extremely effective or it would have become obsolete! Sclerotherapy remains the gold standard in the treatment of spider veins, in spite of the hundreds of lasers introduced to the market. After several treatments, most patients can expect a 50-90% improvement in their veins, though it is possible for new vessels to develop in the same general area. For that reason, it is wise to wear a compression hose at appropriate times if you are prone to the development of spider veins as part of a prevention plan.
Insurance coverage varies, but if the treatment is for cosmetic purposes, most insurance plans will not cover it. You should check with your plan before deciding on the treatment if this is a concern.
Even with the most highly experienced physician performing the injections, there are some possible side effects. These include:
You should speak to your physician if you have a history of either of these, or of a known genetic clotting problem.
While different physicians advocate different post-treatment protocols, the one that has yielded the best results for us over 25-plus years has been the use of a prescription compression hose immediately after the injections and for up to a week afterward. We recommend that you wear these hose indefinitely on long airplane or car trips, as well. Generally, small cotton balls are placed on the treated vessel as soon as the injection is done, to help with compression and thereby disappearance of the vessel. You can resume regular exercise right away, although we advise wearing the compression hose during activity for the first week.
Our board-certified dermatologists are here to help. Contact Gendler Dermatology today at (212) 288-8222 to schedule a consultation.
Make your skin a priority with our leading Upper East Side Medical and Cosmetic Board-Certified Dermatologists.
Book Now